Key Takeaways
- Your sinuses help air move, drain mucus and support clear nose breathing.
- Clear breathing depends on open sinus drainage paths and steady mucus flow.
- Tiny hairs move mucus out of the sinuses before it gets thick.
- Nose breathing warms, moistens and filters air before it reaches your lungs.
- Saline rinsing can help thick mucus move when sinuses feel blocked.
Sinus Basics
Sinus Air Spaces
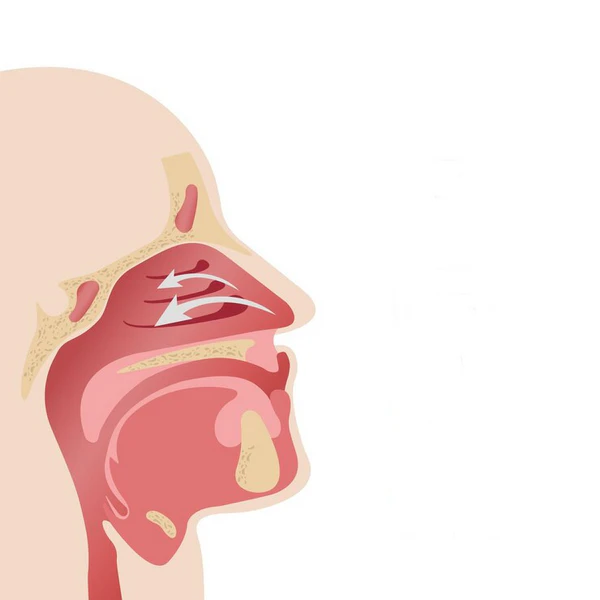
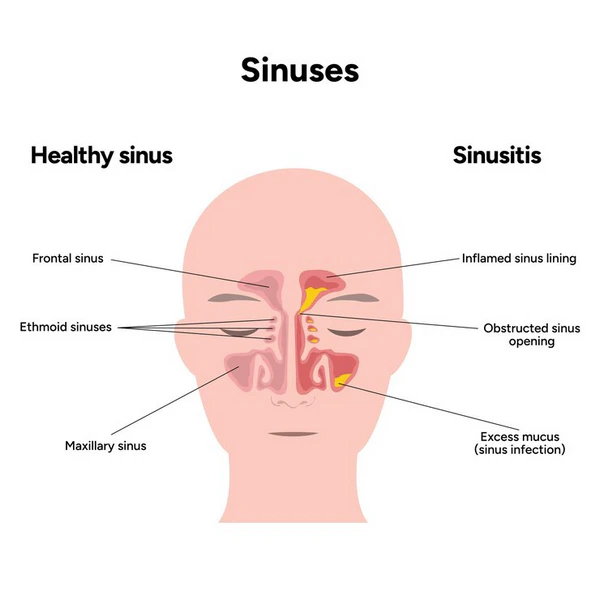
Your sinuses are small air spaces inside the bones around your nose, cheeks, eyes and forehead. They connect to the nose through narrow drainage paths. These paths need to stay open so air can move and mucus can drain. A review on nose and sinus lining describes the nose and sinuses as one linked airway system with shared mucus, immune defense and drainage work (1).
Sinuses are not empty holes with no purpose. They sit inside a living airway surface that makes mucus and moves it toward the nose. That movement keeps the lining cleaner and helps carry out dust, germs and irritants. Clear breathing depends on this steady flow more than most people realize.
Nose Airflow
Your nose does more than let air pass in and out. It warms the air, adds moisture and filters particles before the air reaches your lungs. The nasal cavity supports breathing, smell, air conditioning and immune defense (2).
Nose airflow changes during the day. One side may feel more open while the other side feels tighter. This can be normal because the nose has blood rich tissue that swells and shrinks in cycles. Trouble starts when swelling blocks both sides, thick mucus sits in place or sinus drainage paths stay closed too long.
Breathing through the mouth skips much of this nose work. Dry air reaches the throat more easily. The mouth can feel dry, sleep can feel worse and the nose can get less normal airflow. Clear breathing starts with a nose that can warm, wet and filter air.
Sinus Drainage
Sinus drainage depends on small openings between the sinuses and the nose. These openings are easy to block because they are narrow. Swollen tissue, thick mucus, smoke, dust and dry air can slow the flow. Mucus should move out slowly through the nose and throat. You should not feel it most of the time. When mucus gets thick or the lining gets swollen, pressure can build around the cheeks, eyes or forehead.
Mucus & Movement
Mucus Is Useful
Mucus is not just waste. It traps dust, pollen, smoke particles and germs before they move deeper into the airway. It also keeps the airway lining moist enough to work well.
The problem is stuck mucus, not mucus itself. Thick mucus can sit inside the nose and sinuses when air is dry, the lining is irritated or drainage paths are tight. Once mucus sits too long, breathing feels blocked and pressure can build.
Good sinus care should help mucus move. Harsh drying, heavy fragrance and smoke exposure can work against that goal. The better goal is steady moisture and easy drainage.
Tiny Hairs Move Mucus
Tiny moving hairs called cilia line the nose and sinus surface. They beat in a steady direction and move mucus toward the throat. A review on sinus mucus clearance describes cilia movement as central to sinus health and chronic sinus problems (3).
Cilia need a wet surface. When the surface gets too dry, mucus gets thick and the cilia cannot move it well. Cold dry air, smoke, dust and harsh scents can make this worse. Cilia also need time. If mucus has been stuck for days, one rinse or one steamy shower may not clear everything at once. Steady support works better than aggressive blowing or harsh drying. Nose blowing should be gentle. Hard blowing can push pressure into the ears and can make sore tissue feel worse. Clear one side at a time with light pressure.
Nitric Oxide & Air
Sinus Gas
Your sinuses make nitric oxide, a gas involved in airway defense and normal breathing biology. The paranasal sinuses can act as a large source of nitric oxide for the nasal airway (4).
Nose breathing helps pull this gas through the nasal passages. Mouth breathing does not use the nose in the same way. That is one reason clear nasal airflow is more than comfort.
Nitric oxide also has antimicrobial effects in the airway. Older review work described high nitric oxide levels in the nose and sinuses as part of first line defense against microbes (5). This does not mean nitric oxide is a magic cure. It means the nose has built in chemistry that works best when air can move through it.
Humming Effect
Humming can move air inside the nose and sinuses in a different way than quiet breathing. One study found that humming caused a large rise in nasal nitric oxide output compared with quiet exhalation (6). Humming may help some air movement for a short time.
It is a low risk tool when done gently, but it should not replace proper care when pain, fever or long lasting blockage appears. Try a few slow hums through the nose only when the nose is open enough to move air. Stop if it causes pressure or pain. The goal is easy airflow, not force.
Clear Breathing Support
Moist Air
Dry air can make mucus thicker. Moist air helps the nose lining stay wet enough for mucus movement. A warm shower, clean humidifier or bowl of steam can loosen thick mucus for some people. Humidifiers must stay clean. Dirty water tanks can spread irritants into the air.
Use clean water, wash the tank often and keep indoor air from getting damp enough to grow mold. Air quality also counts. Smoke, strong scent, dust and chemical sprays can irritate the nose lining. The cleaner the air, the less the sinus lining has to defend itself.
Saline Rinsing
Saline rinsing uses salt water to wash the nose and help mucus move. It can be useful when mucus is thick or the nose feels clogged. A Cochrane review found that large volume saline irrigation may help chronic sinus symptoms, while small mist sprays were less useful (7).
Use sterile, distilled or previously boiled water for rinses. Tap water can carry organisms that do not belong inside the nose. Let boiled water cool before use. Do not make the rinse too strong. A harsh salt mix can burn and make the nose feel worse. Use a clean bottle or pot and wash it after each use. Saline should support drainage, not punish the tissue. Stop if rinsing causes pain, ear pressure or bleeding. Seek care if symptoms are severe or keep coming back.
Sleep Position
Sleep can change sinus drainage. Lying flat may make congestion feel worse because blood flow and mucus shift in the nose. A slightly raised head can help some people breathe more easily at night. Side sleeping can also change which nostril feels open. If one side blocks, turning to the other side may help air move. This is not a cure for chronic sinus trouble, but it can help sleep feel easier. Mouth taping should be handled with caution. It is not wise when the nose is blocked, breathing feels hard or sleep apnea is possible. Clear nasal breathing must come first.
For any health concerns or questions about a medical condition, get guidance from a physician or another appropriately trained clinician. Before changing your diet, supplements or health routine, talk with a licensed healthcare professional.
FAQs
Are Sinuses Supposed To Make Mucus?
Yes. Sinuses and the nose make mucus to trap dust, pollen and germs. The problem starts when mucus gets thick, sits too long or cannot drain through the normal paths.
Does Nose Breathing Help Sinuses?
Nose breathing helps air move through the nasal passages and supports normal airway work. It warms, moistens and filters air before it reaches the lungs. Mouth breathing skips much of that work.
Can Saline Rinses Clear Sinuses?
Saline rinses can help thick mucus move, especially when the rinse volume is large enough. Use sterile, distilled or boiled cooled water. Stop if rinsing causes pain, bleeding or ear pressure.
Does Humming Help Sinus Pressure?
Humming may move air inside the nose and raise nasal nitric oxide for a short time. It may feel helpful when the nose is partly open. It should not be forced through blocked or painful sinuses.
When Should Sinus Symptoms Be Checked?
Get checked when sinus pain is severe, symptoms last a long time or fever appears. Also get care for face swelling, vision changes, repeated nosebleeds or breathing that feels unsafe.
Research
Beule, A.G. 2011. Physiology and pathophysiology of respiratory mucosa of the nose and the paranasal sinuses. GMS Current Topics in Otorhinolaryngology Head and Neck Surgery. PMID 22073111.
Freeman, S.C. et al. 2023. Physiology, Nasal. StatPearls. PMID 30252340.
Cohen, N.A. 2006. Sinonasal mucociliary clearance in health and disease. Annals of Otology, Rhinology & Laryngology Supplement. PMID 17040014.
Lundberg, J.O. 2008. Nitric oxide and the paranasal sinuses. Anatomical Record. DOI 10.1002/ar.20782. PMID 18951492.
Djupesland, P.G. et al. 1999. Nitric oxide in the nose and paranasal sinuses, respiratory tract and beyond. Acta Oto Laryngologica. PMID 10613100.
Weitzberg, E. and Lundberg, J.O.N. 2002. Humming greatly increases nasal nitric oxide. American Journal of Respiratory and Critical Care Medicine. DOI 10.1164/rccm.200202 138BC. PMID 12119224.
Chong, L.Y. et al. 2016. Saline irrigation for chronic rhinosinusitis. Cochrane Database of Systematic Reviews. DOI 10.1002/14651858.CD011995.pub2. PMID 27115216.
Phillips, P.S. et al. (2011) ‘Nasal nitric oxide and sinonasal disease: a systematic review of published evidence’, Otolaryngology–Head and Neck Surgery. DOI: 10.1177/0194599810392667. PMID: 21634057.
Lundberg, J.O., Settergren, G., Gelinder, S., Lundberg, J.M., Alving, K. and Weitzberg, E. (1996) ‘Inhalation of nasally derived nitric oxide modulates pulmonary function in humans’, Acta Physiologica Scandinavica. DOI: 10.1046/j.1365-201X.1996.557321000.x. PMID: 8971255.
Imada, M., Nonaka, S., Kobayashi, Y. and Iwamoto, J. (1996) ‘Measurement of nitric oxide in human nasal airway’, European Respiratory Journal. DOI: 10.1183/09031936.96.09030556. PMID: 8730019.
Lindberg, S., Cervin, A. and Runer, T. (1997) ‘Low levels of nasal nitric oxide correlate to impaired mucociliary function in patients with Kartagener’s syndrome’, Acta Oto-Laryngologica. DOI: 10.3109/00016489709113468. PMID: 9349871.
Runer, T. and Lindberg, S. (1998) ‘Effects of nitric oxide on blood flow and mucociliary activity in the human nose’, Annals of Otology, Rhinology & Laryngology. DOI: 10.1177/000348949810700108. PMID: 9439387.
Kirihene, R.K.D.R.A., Rees, G. and Wormald, P.-J. (2002) ‘The influence of the size of the maxillary sinus ostium on the nasal and sinus nitric oxide levels’, American Journal of Rhinology. DOI: 10.1177/194589240201600508. PMID: 12422970.
Törnberg, D.C.F. et al. (2002) ‘Nasal and oral contribution to inhaled and exhaled nitric oxide: a study in tracheotomized patients’, European Respiratory Journal. DOI: 10.1183/09031936.02.00273502. PMID: 12030725.
Maniscalco, M., Weitzberg, E., Sundberg, J., Sofia, M. and Lundberg, J.O. (2003) ‘Assessment of nasal and sinus nitric oxide output using single-breath humming exhalations’, European Respiratory Journal. DOI: 10.1183/09031936.03.00017903. PMID: 12952268.
Jones, N. (2001) ‘The nose and paranasal sinuses physiology and anatomy’, Advanced Drug Delivery Reviews. DOI: 10.1016/S0169-409X(01)00172-7. PMID: 11516776.
Djupesland, P.G., Chatkin, J.M., Qian, W. and Haight, J.S. (2001) ‘Nitric oxide in the nasal airway: a new dimension in otorhinolaryngology’, American Journal of Otolaryngology. DOI: 10.1053/ajot.2001.20700. PMID: 11172211.
Van Cauwenberge, P., Sys, L., De Belder, T. and Watelet, J.B. (2004) ‘Anatomy and physiology of the nose and the paranasal sinuses’, Immunology and Allergy Clinics of North America. DOI: 10.1016/S0889-8561(03)00107-3. PMID: 15062424.
Cole, P. (1998) ‘Physiology of the nose and paranasal sinuses’, Clinical Reviews in Allergy & Immunology. DOI: 10.1007/BF02739327. PMID: 9561336.
Watelet, J.B. and Van Cauwenberge, P. (1999) ‘Applied anatomy and physiology of the nose and paranasal sinuses’, Allergy. DOI: 10.1111/j.1398-9995.1999.tb04402.x. PMID: 10565476.
Spector, B.M., Shusterman, D.J. and Zhao, K. (2023) ‘Nasal nitric oxide flux from the paranasal sinuses’, Current Opinion in Allergy and Clinical Immunology. DOI: 10.1097/ACI.0000000000000871. PMID: 36373691.