Key Takeaways
- Sinusitis means swollen sinus and nasal lining with blocked drainage.
- Most short sinus infections start after a cold and often improve with time.
- Long lasting sinusitis can involve swelling, poor mucus flow, irritants or polyps.
- Salt water rinsing, steam, clean air, sleep and real food can support healing.
- Eye swelling, vision changes, confusion, severe headache or high fever need urgent care.
Sinus Basics
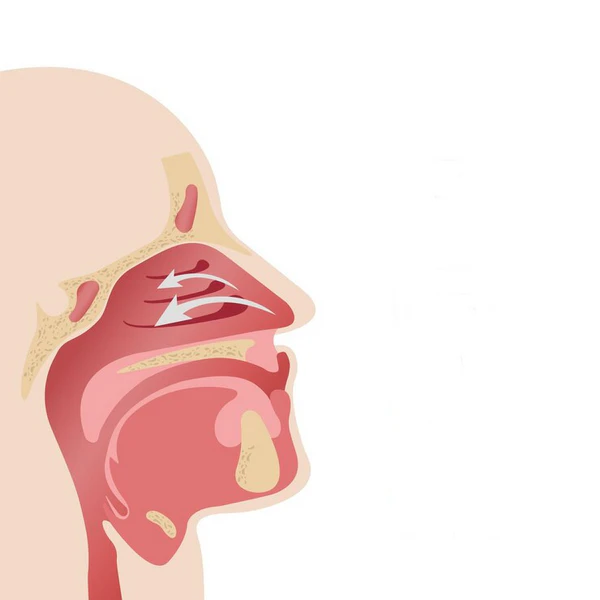
Sinus Drainage
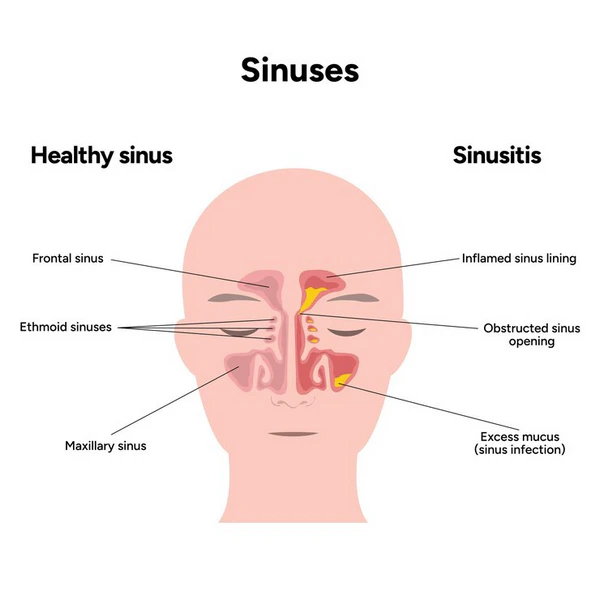
Sinuses are air spaces inside the bones of the face and skull. They sit near the nose, eyes, cheeks and forehead. The sinus lining makes mucus, and tiny moving hairs push that mucus toward the nose. Good mucus flow helps clear dust, germs and irritants before they sit too long.
Sinusitis means the nose and sinus lining has become swollen. Doctors often use the word rhinosinusitis because the nose and sinuses usually react together. Acute sinusitis lasts less than four weeks. Chronic sinusitis lasts twelve weeks or longer (1, 2).
Blocked drainage is the main problem. Swollen lining narrows the small sinus openings. Mucus thickens, pressure rises and breathing through the nose can feel harder. A small drainage problem can feel large because the sinuses sit close to nerves, teeth, eyes and the forehead.
Common Symptoms
Sinusitis can cause stuffy nose, thick mucus, facial pressure, reduced smell, cough, bad breath, ear pressure, upper tooth pain and tiredness. Symptoms can shift during the day because drainage changes with sleep, head position, room air and movement. Fever can happen in short illness, though many people with chronic sinusitis do not have fever.
Facial pressure alone does not prove sinusitis. Migraine, tooth trouble, jaw tension and nerve pain can all feel like sinus pain. Thick drainage and blocked nose make sinusitis more likely. Severe one sided pain, eye swelling or vision changes need fast medical care.
Main Causes
Viral Colds
Most short sinus infections start after a viral cold. The nose lining swells, mucus thickens and sinus openings drain poorly. A major guideline describes viral upper respiratory infection as the most common cause of acute rhinosinusitis (3). The body often clears this with time and basic support.
Mucus color can mislead people. Yellow or green mucus can happen when immune cells are active. Color alone does not prove a bacterial infection. A short cold with congestion, pressure and thick mucus often improves as swelling goes down.
Symptoms that last more than ten days without improvement, worsen after initial improvement or come with strong fever and severe face pain deserve closer care. Those signs can point toward a bacterial shift or a more serious course. Time pattern says more than mucus color.
Long Swelling
Chronic sinusitis is a long lasting swelling problem. It can involve poor mucus flow, immune changes, allergy, irritants, microbes, nasal polyps or blocked anatomy. A 2023 review describes chronic rhinosinusitis as a long term inflammation problem of the nasal and sinus lining (4). One name can cover many different body states.
Some people have nasal polyps. These are soft tissue growths inside the nose that can block airflow and smell. Others have no polyps but still have thick lining, poor drainage and pressure. A nasal exam or scan can help when symptoms keep coming back or last for months.
Air & Irritants
Dry air, smoke, dust, mold, strong odors, pollution and chemical sprays can irritate the nose lining. Irritated lining can swell and make mucus thicker. Indoor air often becomes worse with closed windows, air conditioning, damp rooms or poor cleaning. A nose that is already inflamed can react strongly to small exposures.
Mold deserves special attention because damp rooms can keep the nose and sinuses irritated for months. Cleaning visible mold helps, but moisture control matters more. Leaks, damp walls and poor airflow keep the problem active. A sinus plan fails when the same air keeps irritating the lining every day.
Dental problems can also feed sinus symptoms, especially on one side. Upper back teeth sit close to the maxillary sinuses in the cheeks. A dental infection, failed root canal or hidden tooth problem can irritate the nearby sinus. One sided cheek pressure or foul drainage should raise this question.
Mucus Flow
Cilia Movement
The nose and sinuses rely on tiny moving hairs called cilia. Cilia move mucus toward the throat and nose so the body can clear it. A review on nose and sinus lining describes this mucus system as a core defense for the airway (5). Slow cilia movement can leave mucus sitting too long.
Good mucus needs the right texture. Very thick mucus is harder to move. Dry rooms, low fluid intake, mouth breathing and irritants can make mucus feel sticky. Warm steam may loosen mucus for short relief. Salt water rinsing can help move mucus and wash out irritants.
Nose Breathing
Nose breathing warms, filters and moistens air before it reaches the lungs. Mouth breathing skips much of that work. A blocked nose can push a person toward mouth breathing, and mouth breathing can make the nose and throat feel drier. Dry lining can make mucus harder to clear.
Sleep position can change sinus drainage. Some people feel worse lying flat because mucus pools or swelling increases. Raising the head slightly may help during a short illness. Side sleeping can also change which nostril feels more open.
Natural Support
Salt Water Rinses
Salt water rinsing can help clear mucus, crusts, pollen, dust and irritants from the nose. A clinical guideline supports nasal irrigation for chronic rhinosinusitis because it can improve symptoms and help clear the nasal passages (6). The rinse should feel gentle, not burning or harsh.
Water safety is vital. Use distilled water, sterile water or boiled water that has cooled. Dirty tap water should not go into the nose because rare but serious infections can happen. The bottle or pot also needs washing and drying between uses.
Salt balance matters. Too much salt can burn. Too little can also feel irritating. Premixed packets are often easier than guessing. A gentle rinse once daily during symptoms may be enough for many people, though response varies.
Steam & Humidity
Warm steam can loosen thick mucus and make breathing feel easier for a short time. A warm shower, humid room or careful steam bowl can help when congestion feels dry and stuck. Steam should be warm, not scalding. Burns are a real risk with boiling water.
Room humidity should stay balanced. Very dry air can irritate the nose. Very damp air can feed mold and dust mites. A clean humidifier may help in dry rooms, but a dirty humidifier can blow irritants into the air. Clean equipment matters as much as moisture.
Clean Air
Clean air reduces the daily load on the nose lining. Avoid smoke, scented sprays, strong cleaning fumes and heavy dust when sinus symptoms are active. Vacuuming with a good filter, washing bedding and fixing damp areas can lower indoor irritants. Air cleaning may help when outdoor pollution or indoor dust is high.
Outdoor air can also trigger symptoms. Wind, pollen, smoke and traffic pollution can irritate the nose. Rinsing after heavy exposure can remove some particles before bed. Clean air support is often boring, but it can make a large difference when symptoms keep returning.
Food & Body Support
Lower Sugar Load
High sugar and starch intake can work against steady immune function and blood sugar control. Bread, cereal, desserts, sweet drinks and snack foods also displace better foods. When the body is fighting swelling and mucus buildup, it needs repair nutrients and stable energy. Repeated sugar hits are a poor trade.
Meals based on meat, eggs, seafood, butter, ghee, tallow and broth give protein, animal fat, salt and minerals without a large sugar load. Protein supports tissue repair and immune cells. Animal fat gives long fuel. Salted broth can help when appetite is low and mucus feels thick.
Dairy response varies. Some people tolerate goat milk, yogurt or kefir well. Others feel more mucus or congestion with dairy, especially during a flare. The direct test is simple enough. Remove the suspect food for a short period, then reintroduce it and watch breathing, drainage and throat clearing.
Sleep & Recovery
Sleep gives the body time to repair the lining and control inflammation. Poor sleep can raise stress hormones and weaken immune response. Congestion often makes sleep worse, so the cycle can feed itself. A warm shower, salt rinse and darker room can help the body settle.
Alcohol can worsen nasal swelling and sleep quality for many people. Late sweet foods can also worsen blood sugar swings and make sleep lighter. A real evening meal with protein, fat and salt is usually a better choice than snacks. The body clears mucus better when sleep and fuel are steady.
Sunlight & Movement
Light movement can help mucus move. Walking, gentle chores and outdoor light can make breathing feel more open. Sitting all day can make congestion feel heavier. Movement does not need to be hard to help circulation and drainage.
Sunlight also helps daily rhythm. Morning light tells the body it is daytime and supports sleep timing later. Better sleep helps immune function and repair. Fresh outdoor air can help when the environment is clean, though smoke or heavy pollen may make symptoms worse.
Warning Signs
Urgent Symptoms
Sinus infections can rarely spread near the eye or brain. Eye swelling, eye pain, vision changes, double vision, severe headache, stiff neck, confusion, repeated vomiting, high fever or swelling around the forehead need urgent medical care. Reviews describe orbital and brain complications as medical emergencies (7).
Children need extra caution because symptoms can worsen quickly. Swelling around one eye, trouble moving the eye or a child who looks very ill should be checked fast. Adults with weak immune systems also need earlier care. Serious symptoms should never be watched at home for days.
Long Symptoms
Symptoms lasting twelve weeks or more need a deeper look. Chronic sinusitis can lower smell, sleep, energy and daily function. A clinician may need to check for polyps, allergy, dental causes, immune problems or anatomy that blocks drainage. A scan or nasal scope may be needed when the cause stays unclear.
Repeated short infections also deserve attention. Frequent flares may point to poor mucus flow, indoor air problems, dental disease, mold exposure or immune strain. Treating each flare as a random event can miss the bigger cause. The better path is to look for the reason drainage keeps failing.
Sinusitis is usually a drainage and swelling problem. Short cases often start after a cold and improve with time. Long cases need more investigation. Salt water rinsing, steam, clean air, lower sugar meals, enough sleep and real food can support the body while the deeper cause is addressed.
For any health concerns or questions about a medical condition, get guidance from a physician or another appropriately trained clinician. Before changing your diet, supplements or health routine, talk with a licensed healthcare professional.
FAQs
What Causes Sinusitis?
Sinusitis often starts after a viral cold. Other causes include allergies, irritants, mold, nasal polyps, poor mucus flow, dental problems and blocked sinus drainage.
How Long Does Sinusitis Last?
Acute sinusitis lasts less than four weeks. Chronic sinusitis lasts twelve weeks or longer and usually needs a closer look at swelling, drainage and triggers.
Can Salt Water Rinses Help Sinusitis?
Yes. Salt water rinses can help clear mucus, dust and irritants from the nose. Use distilled, sterile or boiled then cooled water.
When Is Sinusitis Serious?
Eye swelling, vision changes, confusion, stiff neck, severe headache, high fever or forehead swelling need urgent medical care. These signs can point to spread beyond the sinuses.
Can Food Affect Sinus Symptoms?
Food can affect blood sugar, inflammation, mucus feel and immune support. Many people do better with lower sugar meals based on meat, eggs, seafood, animal fat and broth.
Research
Kwon, E. et al. 2025. Acute Sinusitis. StatPearls. Available at: https://www.ncbi.nlm.nih.gov/books/NBK547701/
Kwon, E. et al. 2023. Chronic Sinusitis. StatPearls. Available at: https://www.ncbi.nlm.nih.gov/books/NBK441934/
Chow, A.W. et al. 2012. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clinical Infectious Diseases, 54(8), e72 to e112. Available at: https://academic.oup.com/cid/article/54/8/e72/367144
He, Y. et al. 2023. Pathogenesis and treatment of chronic rhinosinusitis from the perspective of sinonasal epithelial dysfunction. Frontiers in Medicine, 10, 1139240. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10149833/
Beule, A.G. 2011. Physiology and pathophysiology of respiratory mucosa of the nose and the paranasal sinuses. GMS Current Topics in Otorhinolaryngology Head and Neck Surgery. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3199822/
Park, D.Y. et al. 2022. Clinical practice guideline nasal irrigation for chronic rhinosinusitis in adults. Clinical and Experimental Otorhinolaryngology, 15(1), pp. 5 to 23. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8901942/
Wagenmann, M. and Naclerio, R.M. 1992. Complications of sinusitis. Journal of Allergy and Clinical Immunology, 90(3), pp. 552 to 554. Available at: https://pubmed.ncbi.nlm.nih.gov/1527349/
Fokkens, W.J. et al. 2020. European position paper on rhinosinusitis and nasal polyps 2020. Rhinology, 58(S29), pp. 1 to 464. Available at: https://pubmed.ncbi.nlm.nih.gov/32077450/
Lam, K. et al. 2015. The etiology and pathogenesis of chronic rhinosinusitis. The Journal of Allergy and Clinical Immunology, 136(5), pp. 1459 to 1473. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC4874491/
Hildenbrand, T. et al. 2024. The diagnosis and treatment of chronic rhinosinusitis. Deutsches Ärzteblatt International. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11741551/
Achilles, N. and Mösges, R. 2013. Nasal saline irrigations for the symptoms of acute and chronic rhinosinusitis. Current Allergy and Asthma Reports, 13(2), pp. 229 to 235. Available at: https://pubmed.ncbi.nlm.nih.gov/23354530/
Cohen, N.A. 2006. Sinonasal mucociliary clearance in health and disease. Annals of Otology, Rhinology and Laryngology Supplement. Available at: https://pubmed.ncbi.nlm.nih.gov/17040014/
Djupesland, P.G. 2013. Nasal drug delivery devices. Characteristics and performance in a clinical perspective. Drug Delivery and Translational Research, 3(1), pp. 42 to 62. Available at: https://pubmed.ncbi.nlm.nih.gov/25786603/
Naraghi, M. et al. 2007. Nitric oxide. A new concept in chronic sinusitis pathogenesis. American Journal of Otolaryngology, 28(5), pp. 334 to 337. Available at: https://pubmed.ncbi.nlm.nih.gov/17826536/
Radovani, P. et al. 2013. Orbital complications of sinusitis. Balkan Medical Journal, 30(3), pp. 265 to 268. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC4115963/