Key Takeaways
- Triglycerides shift after meals, so test timing can change results.
- Many labs use 150 mg per dL as a common cutoff.
- Sugar, starch, plus alcohol can raise triglycerides for many people.
- One to three meals daily can shorten daily blood fat surges.
- Family traits can shape triglycerides even with careful food choices.
What Are Triglycerides
Fuel In The Blood
Triglycerides are a type of fat the body stores for energy, then uses later when food is not coming in. They are made from three fatty acids joined to a glycerol backbone, which is a small structure that holds them together. Blood is water based, so fat needs a way to travel without clumping.
The body solves that by packing triglycerides into tiny carriers called lipoproteins, which are little bundles of fat plus protein that move through the blood. One key carrier is VLDL, which stands for very low density lipoprotein, and the liver makes a lot of it. After a meal, the gut also sends fat into the blood in similar carriers, then the body unloads that fuel into tissues that need it.
Triglycerides often rise after eating, then fall as the body clears those carriers. A detailed review explains how fasting tests, non fasting tests, plus after meal tests each show a different slice of the same system ( Keirns et al., 2021)
Why The Body Stores Them
The body stores extra energy as triglycerides mostly in fat tissue, then releases that energy between meals. Hormones help control this back and forth, which lets people go hours without eating while still having steady fuel.
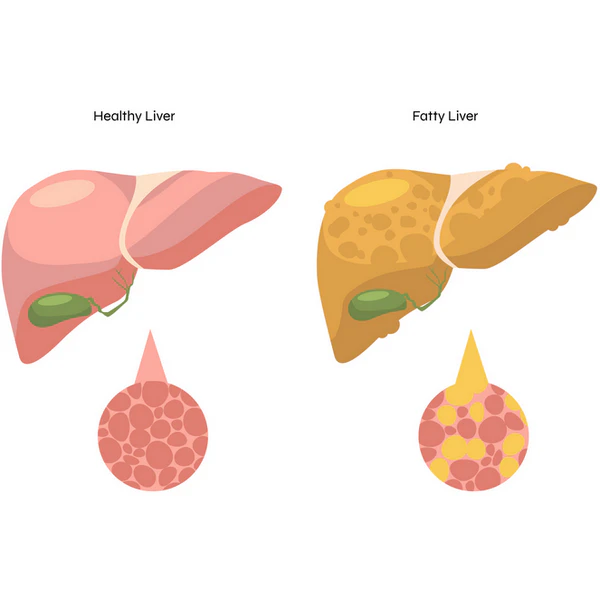
The liver also makes triglycerides when extra energy is coming in, then ships them out in VLDL. When that export stays high for a long time, blood triglycerides can stay high as well, which is one reason the number can reflect how the liver is handling incoming energy.
Fasting Plus Non Fasting Tests
Many clinics ask for fasting before a triglycerides test, which often means no calories for about eight to twelve hours. Fasting reduces the strong meal effect, so the result is easier to compare with earlier fasting tests from the same person.
Non fasting tests can still be useful for screening, because most people spend most hours of the day in a fed state. The same review notes that non fasting values can still relate to health risk in large studies, though the best way to use them depends on the question being asked (Keirns et al., 2021)
How Labs Set Ranges
Common Cutoffs
Most lab reports list triglycerides in mg per dL, though some regions use mmol per L. Many labs group results with cutoffs such as under 150 mg per dL, then higher bands that may be labeled borderline high, high, or very high.
These cutoffs help clinics sort results into broad groups for tracking and record keeping. They do not explain the cause of a result, and they do not replace a full review of food timing, alcohol use, sleep, stress, illness, plus recent activity.
Why One Result Can Mislead
A triglycerides test is a snapshot, and snapshots can be distorted by what happened in the day or two before the blood draw. A late meal can raise the result, then a strict fast can lower it on a different day, even when the person has not changed much overall.
A simple way to get clearer meaning is to keep test conditions similar each time. That can mean fasting each time, doing the draw at a similar hour, plus keeping the day before the test fairly steady. A short note can list last meal time, alcohol intake, sleep hours, plus any illness, because those items can explain a surprising spike without guessing.
Units Without Stress
A number can look very different when the unit changes, so checking the unit printed next to the result helps prevent confusion. Lab portals usually show the unit clearly, and a clinician can explain how the lab flags high results in its own system.
What Raises Triglycerides
Sugar Plus Starch Load
Triglycerides often rise when meals are heavy in sugar and refined starch, because the liver can convert extra carbohydrate energy into fat. A paper on high carbohydrate feeding describes how low fat, high carbohydrate diets can raise plasma triglycerides, and it discusses increased fat making as one reason for the rise (Hudgins, 2000)
A trial in people with type 2 diabetes found that changing the source or amount of dietary carbohydrate changed after meal triglycerides plus after meal glucose responses (Wolever et al., 2013) When carbohydrates are kept low or removed, the liver often has less extra carbohydrate energy to turn into triglycerides. For many people, that means avoiding grains, sweet drinks, desserts, plus most packaged snack foods.
Fiber is often marketed as essential, yet triglycerides can still improve when fiber falls, because triglycerides can respond strongly to carbohydrate load itself. People who feel better with fewer plants can focus on animal foods for nutrient density, because animal foods provide many nutrients in forms the body can use with less work.
Alcohol Effects
Alcohol can raise triglycerides for some people, especially when drinking comes with late eating or sweet mixers. Evidence on alcohol is messy because many studies are observational, and lifestyle differences can distort the picture.
A recent review on alcohol and cardiovascular health describes broad risks with increasing intake across many conditions, while also highlighting how older messages about benefit have not held up well across stronger lines of evidence (Arora et al., 2022)
Meal Timing And Grazing
Triglycerides rise after meals then fall as fats clear from the blood, so frequent eating can keep triglycerides elevated for more hours. A controlled study compared the same calories given as three meals versus six meals in obese women, and meal frequency changed after meal triglycerides plus insulin responses (Heden et al., 2013)
One to three meals daily with no grazing fits well here, because longer gaps give the body time to clear post meal fats. This approach can be easier when meals have enough animal fat, because low fat meals often leave people hungry sooner.
Animal Based Steps That Fit
Meals Built On Animal Fat
Animal fats can support steady energy while keeping carbohydrate low. Many people find that fatty meat, eggs cooked in butter, plus full fat dairy if tolerated can reduce hunger, which makes fewer meals feel natural rather than forced.
A controlled diet study reported lower triglycerides plus higher HDL cholesterol on a high meat diet compared with lower meat diets in that study setting (Hunt et al., 1993) Simple meal ideas can keep this easy. A first meal can be three or four eggs cooked in butter with a serving of beef or lamb. A second meal can be ground beef patties with cheese, or slow cooked meat with salt to taste, then no snacks until the next meal time.
Plant foods contain antinutrients, which are plant defense compounds that can bind minerals or irritate digestion in some people. Grains are a common source of lectins plus phytates, and many people do better when grains are avoided, especially when the goal is lower carbohydrate intake.
“The high meat diet, compared to the low meat or low meat supplemented diets, was associated with higher HDL cholesterol (1.50 vs 1.36 or 1.39 mmol/L, p<0.0005) and lower triglycerides (1.39 vs 1.66 or 1.72 mmol/L, p<0.0003), without change in total or LDL cholesterol.“
(Hunt, Hoverson, Gallagher, & Johnson, 1993)
https://doi.org/10.1016/0002-8223(93)91327-m.
Seed Oils Plus Fortified Foods
Seed oils show up in chips, fries, dressings, plus many restaurant meals. These foods often come with refined starch too, which can drive triglycerides higher for many people.
Fortified foods are also common, especially in grain products, cereals, plus snack bars. Avoiding packaged grain foods often reduces fortified products by default, which fits a focus on whole animal foods rather than factory blends.
Genes And Long Term Tracking
Some people inherit higher triglycerides because of how their bodies clear triglyceride rich particles. A genetics review explains that proving cause in trials is hard because triglycerides move with other lipid markers, yet genetic findings support a meaningful link between triglyceride rich particles plus atherosclerotic disease (Tada and Kawashiri, 2019)
Tracking trends is key for inherited risk. Testing under similar conditions every few months can show whether changes in food, alcohol, plus meal timing are actually shifting the baseline. Very high triglycerides deserve fast clinical review, because extreme levels can raise the risk of acute problems. That is not a place for guesswork or online advice.
Consult a licensed healthcare professional before starting, stopping, or changing any diet, supplement, medication, or wellness practice. For questions about a medical condition or symptoms, seek advice from a qualified clinician who can assess your situation.
FAQs
What are triglycerides in plain language?
Triglycerides are stored fat the body can use for energy between meals, and they travel in blood inside tiny fat carrying particles.
What triglycerides level do labs often call normal?
Many labs use under 150 mg per dL as a common cutoff, though ranges can vary by lab and by test conditions.
Should someone fast before a triglycerides test?
Many clinics prefer fasting because meals can raise triglycerides for hours, though non fasting tests can still help with screening when used consistently.
Why can triglycerides jump from one test to the next?
Late meals, sugar and starch intake, alcohol, poor sleep, illness, stress, plus lower activity can all shift triglycerides quickly.
Can fewer meals per day help triglycerides?
Some people see improvement with one to three meals daily, because longer gaps between meals can reduce time spent in a high post meal state.
Research
Keirns, B.H., Sciarrillo, C.M., Koemel, N.A. and Emerson, S.R. (2021). Fasting, non-fasting and postprandial triglycerides for screening cardiometabolic risk. Journal of Nutritional Science, 10, e75.
Hudgins, L.C. (2000). Effect of High-Carbohydrate Feeding on Triglyceride and Saturated Fatty Acid Synthesis. Proceedings of the Society for Experimental Biology and Medicine, 225(3), 178–183.
Wolever, T.M.S., Gibbs, A.L., Chiasson, J.L., Connelly, P.W., Josse, R.G., Leiter, L.A., Maheux, P., Rabasa-Lhoret, R., Rodger, N.W. and Ryan, E.A. (2013). Altering source or amount of dietary carbohydrate has acute and chronic effects on postprandial glucose and triglycerides in type 2 diabetes: Canadian trial of Carbohydrates in Diabetes (CCD). Nutrition, Metabolism and Cardiovascular Diseases, 23(3), 227–234.
Arora, M., et al. (2022). The Impact of Alcohol Consumption on Cardiovascular Health. Current Cardiology Reports, 24, 1–14.
Heden, T.D., Liu, Y., Sims, L.J., Whaley-Connell, A.T., Chockalingam, A., Dellsperger, K.C. and Kanaley, J.A. (2013). Meal frequency differentially alters postprandial triacylglycerol and insulin concentrations in obese women. Obesity (Silver Spring), 21(1), 123–129.
Hunt, J.R., Hoverson, B.S., Gallagher, S.K. and Johnson, L.K. (1993). Low or high meat consumption: effects on serum lipids, iron, and zinc in women. Journal of the American Dietetic Association, 93(11), 1241–1247.
Tada, H. and Kawashiri, M.A. (2019). Genetic Variations, Triglycerides, and Atherosclerotic Disease. Journal of Atherosclerosis and Thrombosis, 26(2), 128–131.
Kim, J.Y., Lee, K.J., Kang, J., Kim, B.J., Han, M.K., Kang, K. et al. (2022). Fasting and Non-Fasting Triglycerides in Patients With Acute Ischemic Stroke. Journal of Korean Medical Science, 37, e100.
Tada, H., Takamura, M. and Kawashiri, M.A. (2021). Triglycerides on the Rise!. Journal of Atherosclerosis and Thrombosis, 28, 1–3.
Rosenson, R.S., Cushman, M., McKinley, E.C., Muntner, P., Wang, Z., Vaisar, T. et al. (2023). Association Between Triglycerides and Incident Cognitive Impairment in Black and White Adults in the Reasons for Geographic and Racial Differences in Stroke Study. Journal of the American Heart Association, 12, e026833.
Hanif, S., Fatima, S., Nazli, R., Ullah, N. and Zeb, F. (2022). Evaluation Of Triglycerides Levels In Serum And Tears Of Obese And Non-Obese Normal Adult Humans And Its Effects On Pupillary Response. Journal of Ayub Medical College, Abbottabad: JAMC, 34, 1–6.
Semova, I. and Biddinger, S.B. (2021). Triglycerides in Nonalcoholic Fatty Liver Disease: Guilty Until Proven Innocent. Trends in Pharmacological Sciences, 42(3), 183–190.
Vallejo-Vaz, A.J., Corral, P., Schreier, L. and Ray, K.K. (2020). Triglycerides and residual risk. Current Opinion in Endocrinology, Diabetes, and Obesity, 27(2), 95–102.
Dron, J.S. and Hegele, R.A. (2017). Genetics of Triglycerides and the Risk of Atherosclerosis. Current Atherosclerosis Reports, 19, 1–9.
Natto, Z.S., Yaghmoor, W., Alshaeri, H.K. and Van Dyke, T.E. (2019). Omega-3 Fatty Acids Effects on Inflammatory Biomarkers and Lipid Profiles among Diabetic and Cardiovascular Disease Patients: A Systematic Review and Meta-Analysis. Scientific Reports, 9(1), 1–10.
Qin, S., Huang, L., Gong, J., Shen, S., Huang, J., Ren, H. and Hu, H. (2017). Efficacy and safety of turmeric and curcumin in lowering blood lipid levels in patients with cardiovascular risk factors: A meta-analysis of randomized controlled trials. Nutrition Journal, 16, 1–12.
Rafraf, M., Malekiyan, M., Asghari-Jafarabadi, M. and Aliasgarzadeh, A. (2014). Effect of Fenugreek Seeds on Serum Metabolic Factors and Adiponectin Levels in Type 2 Diabetic Patients. International Journal for Vitamin and Nutrition Research, 84(3–4), 196–205.
Yang, J., Wu, L. and Chiu, H. (2018). High-Intensity Intermittent Exercise Increases Fat Oxidation Rate and Reduces Postprandial Triglyceride Concentrations. Nutrients, 10(4), 1–12.
Ullrich, I.H., Peters, P.J. and Albrink, M.J. (1985). Effect of low-carbohydrate diets high in either fat or protein on thyroid function, plasma insulin, glucose, and triglycerides in healthy young adults. Journal of the American College of Nutrition, 4(4), 451–459.
Aviram, M., Brox, J. and Nordoy, A. (1986). Acute Effects of Dietary Cod Liver Oil and Cream on Plasma Lipoproteins. Annals of Nutrition and Metabolism, 30(2), 143–148.
Fatima, F., Memon, A., Zafar, S., Amar, Z., Talpur, A.S., Hashim, S., Maqsood, H., Hafizyar, F. and Kumar, B. (2021). Role of Cod Liver Oil in Reducing Elevated Lipid Parameters. Cureus, 13(6), e15556.
Egeland, G.M., Meyer, H.E., Selmer, R., Tverdal, A. and Vollset, S.E. (2001). Cod Liver Oil Consumption, Smoking, and Coronary Heart Disease Mortality: Three Counties, Norway. International Journal of Circumpolar Health, 60(2), 143–149.
Taylor, A.E., Lu, F., Carslake, D., Hu, Z., Qian, Y., Liu, S., Chen, J. and Smith, G.D. (2015). Exploring causal associations of alcohol with cardiovascular and metabolic risk factors in a Chinese population using Mendelian randomization analysis. Scientific Reports, 5, 14005.
Min, H.S., Kang, J.Y., Sung, J. and Kim, M.K. (2016). Blood Triglycerides Levels and Dietary Carbohydrate Indices in Healthy Koreans. Journal of Preventive Medicine and Public Health, 49(3), 153–164.
Burchard, H.U. and Tischendorf, F.W. (1989). Die Auswirkungen der Einnahme von Lebertran auf den Blutfettspiegel, das Lipoproteinprofil und die Blutungszeit. Zeitschrift für Ernährungswissenschaft, 28(1), 84–91.
Goel, S., Sharma, A. and Garg, A. (2018). Effect of Alcohol Consumption on Cardiovascular Health. Current Cardiology Reports, 20(4), 19.
Hodges, R.E. and Krehl, W. (1965). The Role of Carbohydrates in Lipid Metabolism. The American Journal of Clinical Nutrition, 17(5), 334–346.
Iqbal, M.P. (2014). Trans fatty acids – A risk factor for cardiovascular disease. Pakistan Journal of Medical Sciences, 30(1), 194–197.
McCarty, M.F. (2004). An elevation of triglycerides reflecting decreased triglyceride clearance may not be pathogenic – relevance to high-carbohydrate diets. Medical Hypotheses, 63(6), 1065–1073.
Rosales, C., Gillard, B.K. and Pownall, H.J. (2020). The Alcohol–High-Density Lipoprotein Athero-Protective Axis. Biomolecules, 10(7), 1–20.
Smith, U. (1994). Carbohydrates, fat, and insulin action. The American Journal of Clinical Nutrition, 59(3), 686S–689S.
Truswell, A.S. (1994). Food carbohydrates and plasma lipids””an update. The American Journal of Clinical Nutrition, 59(3), 710S–718S.