Key Takeaways
- Intestinal cells use glutamine heavily during stress to support repair energy and barrier function.
- Permeability studies show mixed results with benefits clearer in specific stress related situations.
- Exercise heat and illness can strain the gut barrier and raise interest in glutamine.
- Trials in irritable bowel syndrome suggest possible symptom help for some people.
- Safety depends on context dose and medical history so individual guidance is sensible.
Intestinal Energy & Repair
Enterocytes Need Fuel
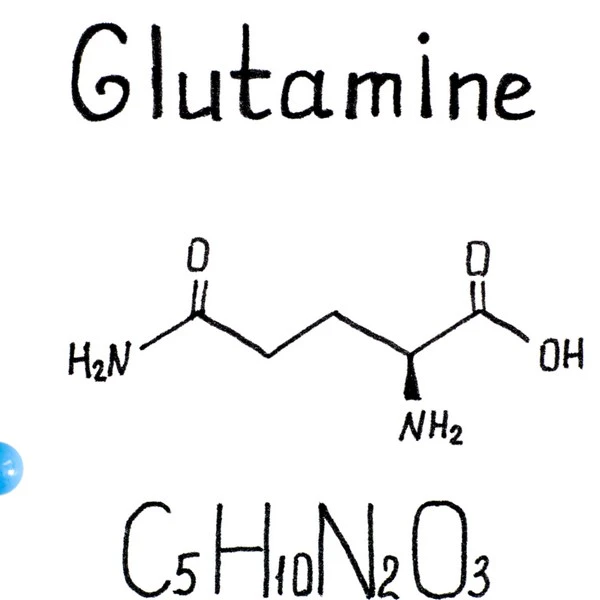
The lining of the small intestine turns over quickly, so it needs steady raw materials and steady energy. Many tissues can lean on glucose or fatty acids, yet intestinal cells often rely heavily on glutamine as a working fuel source.
Research reviews describe glutamine as a key substrate for enterocytes and immune cells in the gut, especially when the gut is under inflammatory or metabolic strain. (1, 2)
Stress changes priorities inside the body, so nutrient traffic shifts toward tissues trying to defend and repair. Infection, heavy training, heat stress, surgery, burns, chemotherapy and prolonged poor sleep can all increase gut stress in different ways.
Glutamine demand can rise in these states, partly because the gut barrier is being challenged while immune activity is ramping up. Reviews in Amino Acids and Current Opinion in Clinical Nutrition and Metabolic Care describe this bench to bedside idea, while also warning that clinical outcomes depend on the situation and the person. (2, 3)
Support For The Barrier
Gut permeability is often described as a proxy for barrier integrity, even though tests vary and do not capture every aspect of barrier function. Tight junction proteins, mucus layers, local blood flow and immune signaling all contribute to whether the barrier stays selective under stress.
Mechanistic papers describe glutamine as influencing tight junction regulation and inflammatory signaling, which helps explain why it gets studied in leaky gut discussions. (2, 1)
A recent systematic review and meta analysis of adult trials focused on gut permeability outcomes and tried to pool evidence across studies that used different stressors different assays and different doses. Meta analyses can clarify trends, yet they also inherit weaknesses from inconsistent protocols and variable trial quality. The review still gives a useful map of where evidence is stronger and where it is thinner. (4)
Stress Loads On The Gut
Heat Exercise
Endurance training can reduce blood flow to the gut during exercise, especially in heat, and this can increase gut symptoms and barrier disruption. Two controlled studies in athletes tested oral glutamine around demanding exercise and measured permeability related markers. Results suggested glutamine reduced permeability markers during running in the heat and influenced tight junction related measures during exercise induced gut stress. (5, 6)
A useful way to read these results is to treat them as stress specific, not as proof of a universal gut fix. Athletes in heat have a clear acute stress model, with predictable physiological strain that can be measured over hours and days.
People with chronic digestive complaints often have more complex drivers including infection history diet triggers sleep disruption and psychological stress, so a single nutrient rarely maps perfectly from an exercise model. Even so, these trials support the idea that glutamine can be relevant when the gut barrier is pushed hard in a short window. (5, 6)
Chronic Gut Strain
Irritable bowel syndrome is a broad diagnosis, so trial results depend heavily on which subgroup is studied and how it is defined. A randomised placebo controlled trial in Gut studied glutamine in postinfectious irritable bowel syndrome, which is a subgroup with a clear trigger event and plausible barrier disruption.
The trial reported benefit for that studied group, which is clinically interesting because it points to a more targeted use case rather than a one size fits all approach. (7) Diet can shift symptoms quickly in IBS, so combined approaches complicate interpretation but can reflect real life use.
A trial in Frontiers in Nutrition studied glutamine added to a low FODMAP diet for IBS management and reported enhanced effects with the combination. Results like this can be read as signal that glutamine may support some people while dietary change reduces fermentable triggers, although the specific study design still shapes what can be concluded. (8)
Clinical Evidence In Disease States
Permeability In Adult Trials
The most careful summary for permeability outcomes is the systematic review and meta analysis focused on adult clinical trials. Evidence suggested glutamine supplementation can influence gut permeability measures in some contexts, yet effects are not uniform across populations and protocols.
The review also underscores a basic issue, gut permeability is not measured the same way across trials, so pooled conclusions can be less stable than people assume when they hear the term meta analysis. (4)
Readers often want a simple answer on whether glutamine seals the gut barrier. The evidence does not support a blanket promise, but it does support further interest in specific stress related settings and specific symptom clusters.
People doing heavy endurance work in heat, people with postinfectious IBS and some hospital settings may be closer to the use cases where glutamine has a clearer rationale. The gap between mechanism and outcomes should stay in view because strong biochemical plausibility does not guarantee meaningful symptom change. (4, 3)
Inflammatory Bowel Disease Trials
Crohns disease has a different biology than IBS, with deeper immune driven inflammation and tissue injury. A randomized controlled trial in Digestive Diseases and Sciences tested glutamine and whey protein in Crohns disease and reported improvements in permeability and morphology measures.
Another double blind randomized trial in a pediatric journal tested a glutamine enriched polymeric diet for active Crohns disease. These studies show serious interest in glutamine within inflammatory bowel disease care, while also reminding you that outcomes vary and formulas differ, so generalization is limited. (9, 10)
Crohns trials also highlight a practical point about real world supplementation. Many interventions in this area occur inside broader nutrition therapy, where calorie intake protein adequacy and disease activity can shift at the same time. Glutamine may be one piece, but it may not be the biggest lever for every patient, especially when medication changes or flare severity dominate the picture. Careful trial reading helps avoid overclaiming. (9, 10)
Use In Real Life
Food Sources & Timing
Glutamine is found in many protein foods, including traditional whole foods many people already eat. People focusing on digestion often do better with simpler meals, with enough protein and fat to stay satisfied without constant snacking.
A one to three meal rhythm can reduce frequent gut stimulation, which may help some people notice whether a supplement is truly helping. Glutamine powders are often taken on an empty stomach, yet studies vary in timing and dose, so personal tolerance and the studied context should guide choices.
Some people reach for glutamine because of gut symptoms after high carbohydrate eating or after highly processed meals. Food quality can influence gut symptoms through additives alcohol sugar alcohols and emulsifiers, so supplement effects can be hard to detect if diet stays chaotic.
A calmer baseline of whole traditional meals can make it easier to judge whether glutamine changes anything noticeable. Trials combining glutamine with diet changes in IBS show how diet can be part of the response, even when the study goal is to test a supplement. (8)
Safety & Oversight
Safety discussions should separate supplement regulation from clinical evidence. The US Food and Drug Administration describes how dietary supplements are regulated differently than drugs and how quality varies across brands. People often assume a powder is automatically safe, yet quality control and labeling accuracy are practical concerns. (11)
Medical reference sources list potential side effects and caution areas, including that people with certain medical conditions should involve a clinician. Memorial Sloan Kettering also summarizes glutamine use in integrative care and notes interactions and safety considerations in cancer settings.
These references do not replace individualized care, but they can help you frame risk, especially if you have liver or kidney disease a complex medication list or an active cancer treatment plan. (12, 13)
A sensible standard is to treat glutamine as situation specific rather than routine forever. People with exercise related gut distress may use it around training blocks. People with postinfectious IBS may test it for a defined period while tracking symptoms, stool changes and food tolerance. Clinical trial durations vary, so copying a protocol from a different population can lead to wasted effort or missed warning signs. (7, 4)
For any health concerns or questions about a medical condition, get guidance from a physician or another appropriately trained clinician. Before changing your diet, supplements or health routine, talk with a licensed healthcare professional.
FAQs
Can glutamine help with leaky gut?
Some studies report improvements in permeability related measures in certain settings, yet results are not uniform across all groups. Many trials use different tests and different stress models, so the best interpretation is that glutamine can help in some contexts rather than being a universal fix.
Is glutamine useful for postinfectious IBS?
A controlled trial in postinfectious IBS reported benefit in the studied group. Postinfectious IBS is a more specific subgroup than general IBS, so results may not apply to everyone with an IBS label.
Does glutamine help athletes with stomach issues during training?
Studies in endurance exercise stress models suggest glutamine can reduce permeability markers during demanding sessions, especially in heat. Training load hydration and meal timing still influence symptoms strongly, so glutamine is usually one part of a broader plan.
How long should someone try glutamine before deciding?
Trials often run for weeks, not days, and effects can be subtle. A defined trial period with consistent diet and routine helps you judge changes more clearly than casual use.
Are there people who should avoid glutamine?
People with complex medical conditions or active cancer treatment should involve a clinician before starting. People with kidney or liver disease or a complicated medication list also benefit from professional guidance.
Research
Kim, M.H. and Kim, H. (2017) The roles of glutamine in the intestine and its implication in intestinal diseases. International Journal of Molecular Sciences, 18(5), p. 1051. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5454963/
Wang, B., Wu, G., Zhou, Z., Dai, Z., Sun, Y., Ji, Y., Li, W., Wang, W., Liu, C., Han, F., Wu, Z. and Wang, J. (2015) Glutamine and intestinal barrier function. Amino Acids, 47(10), pp. 2143–2154. Available at: https://pubmed.ncbi.nlm.nih.gov/24965526/
Achamrah, N., Déchelotte, P. and Coëffier, M. (2017) Glutamine and the regulation of intestinal permeability from bench to bedside. Current Opinion in Clinical Nutrition and Metabolic Care, 20(1), pp. 86–91. Available at: https://pubmed.ncbi.nlm.nih.gov/27749689/
Abbasi, F., Mahdavi, R., Nikniaz, Z., Moludi, J., Faramarzi, E. and Nikniaz, L. (2024) A systematic review and meta analysis of clinical trials on the effects of glutamine supplementation on gut permeability in adults. Amino Acids, 56(1), p. 60. Available at: https://pubmed.ncbi.nlm.nih.gov/39397201/
Pugh, J.N., Sage, S., Hutson, M., Doran, D.A. and Fleming, S.C. (2017) Glutamine supplementation reduces markers of intestinal permeability during running in the heat in a dose dependent manner. European Journal of Applied Physiology, 117(12), pp. 2569–2577. Available at: https://pubmed.ncbi.nlm.nih.gov/29058112/
Zuhl, M.N., Lanphere, K.R., Kravitz, L., Mermier, C.M., Schneider, S., Dokladny, K. and Moseley, P.L. (2014) Effects of oral glutamine supplementation on exercise induced gastrointestinal permeability and tight junction protein expression. Journal of Applied Physiology, 116(2), pp. 183–191. Available at: https://pubmed.ncbi.nlm.nih.gov/24285149/
Zhou, Q., Verne, M.L., Fields, J.Z., Lefante, J.J., Basra, S., Salameh, H. and Verne, G.N. (2019) Randomised placebo controlled trial of dietary glutamine supplements for postinfectious irritable bowel syndrome. Gut, 68(6), pp. 996–1002. Available at: https://pubmed.ncbi.nlm.nih.gov/30108163/
Rastgoo, S., Ebrahimi Daryani, N., Agah, S., Hekmatdoost, A. and Poustchi, H. (2021) Glutamine supplementation enhances the effects of a low FODMAP diet in irritable bowel syndrome management. Frontiers in Nutrition, 8, 746703. Available at: https://pubmed.ncbi.nlm.nih.gov/34977110/
FDA (2022) FDA 101 Dietary supplements. U.S. Food and Drug Administration. Available at: https://www.fda.gov/consumers/consumer-updates/fda-101-dietary-supplements
MedlinePlus (2017) L glutamine drug information. U.S. National Library of Medicine. Available at: https://medlineplus.gov/druginfo/meds/a617035.html
MSK (2024) Glutamine. Memorial Sloan Kettering Cancer Center. Available at: https://www.mskcc.org/cancer-care/integrative-medicine/herbs/glutamine
Benjamin, J., Makharia, G., Ahuja, V., Anand Rajan, K.D., Kalaivani, M., Gupta, S.D., Joshi, Y.K. and Ramakrishna, B.S. (2012) Glutamine and whey protein improve intestinal permeability and morphology in patients with Crohns disease a randomized controlled trial. Digestive Diseases and Sciences, 57(4), pp. 1000–1002. Available at: https://pubmed.ncbi.nlm.nih.gov/22038507/
Akobeng, A.K., Miller, V., Stanton, J., Elbadri, A.M., Thomas, A.G. and Thomas, P.W. (2000) Double blind randomized controlled trial of glutamine enriched polymeric diet in the treatment of active Crohns disease. Journal of Pediatric Gastroenterology and Nutrition, 30(1), pp. 78–84. Available at: https://pubmed.ncbi.nlm.nih.gov/10630444/