Key Takeaways
- The heart works without pause, so it needs steady fuel, oxygen, and minerals daily.
- Heart cells hold many mitochondria, which are tiny parts that make usable cell energy.
- Sodium, potassium, and magnesium help support rhythm, pulse control, and recovery after effort.
- Sugar swings, poor sleep, stress, and stimulants can make daily heart function feel less steady.
- Simple meals, easy walks, and fewer eating times often support calmer heart output.
Heart Work
Busy Cell Design
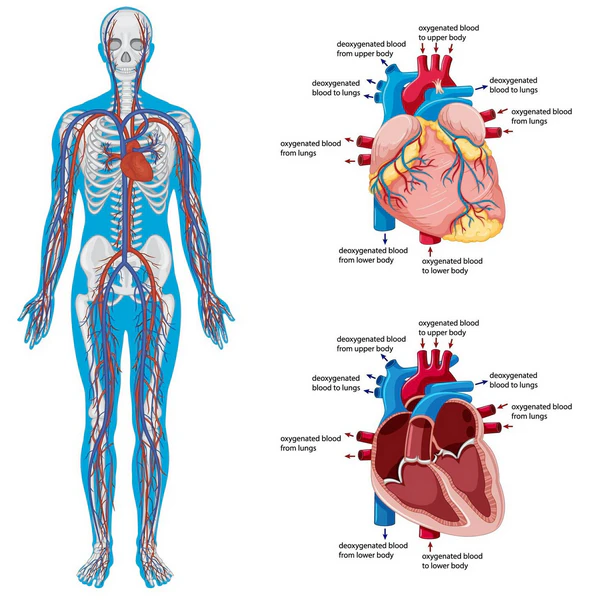
The heart never gets a true rest period, because it keeps beating through sleep, work, worry, meals, heat, and movement. Most muscles stop and start through the day, but the heart keeps working without pause from birth to death.
That nonstop workload helps explain why small strains can feel large in the chest. A poor night of sleep, low food intake, or a long day of pressure can show up fast as a pounding pulse, short breath, or a flutter feeling.
Heart muscle cells are built for that constant job, and they contain large numbers of mitochondria, which are tiny parts inside cells that turn fuel into usable energy.
Research on heart cell design and metabolism shows how strongly the heart depends on a constant energy supply (Balaban, 2012; Li et al., 2023).
Fat Based Fuel
The healthy heart can use more than one fuel, but it leans heavily on fatty acids during rest and steady work.
Reviews of cardiac metabolism describe fatty acid oxidation as a major energy source, while more glucose use tends to show up in stress states and failing states (Stanley et al., 2005; Lopaschuk et al., 2021).
That point helps explain why many people feel less steady on a day built around cereal, toast, juice, snack bars, and sweet drinks. Fast fuel can drive fast swings, and the chest may feel those swings before the mind finds words for them.
A steadier setup often starts with animal foods that bring dense fuel and well used nutrients. Eggs, beef, lamb, sardines, shellfish, butter, broth, and full fat dairy if tolerated can give protein, fat, copper, and minerals in a form the body can use well.
Core Needs
Oxygen Supply
The heart runs best on steady oxygen based energy, so oxygen delivery deserves more respect than it usually gets. Calm breathing, decent blood flow, enough rest, and enough fuel all help that process stay smooth.
When oxygen delivery falls, the heart may beat harder or faster to keep output up. A person may notice that as getting winded on easy walking, feeling chest effort too soon, or taking too long to settle after simple activity.
That does not prove heart disease by itself, but it does show strain that deserves attention. Easy walking can act like a clear mirror, because calm walking should not leave a healthy person gasping unless base fitness, recovery, or stress load is poor. Copper supports oxygen based energy steps in the body.
Mineral Flow
Each beat depends on electrical signals, and those signals rely on mineral balance. Sodium and potassium help set the charge across heart cells, while magnesium helps the system fire and reset in a calmer way.
Research on low magnesium and abnormal heart rhythms suggests that magnesium shortfalls can raise rhythm trouble in some settings (Negru et al., 2022).
Research on potassium shifts shows that low potassium can also disturb heart rhythm and recovery after each beat (Weiss et al., 2017; Tazmini et al., 2020).
Copper deficiency is bad for the heart because copper helps the body make energy, handle iron, and support normal heart muscle function.
When copper status or ceruloplasmin function is poor, iron handling can break down, and that may contribute to heart muscle damage or iron buildup in the heart (Collins, Prohaska and Knutson, 2010; Medeiros, Davidson and Jenkins, 1993; Liu and Miao, 2022).
Food, sweat, alcohol, heat, poor sleep, and stress can all shift this balance. Some people notice the problem when standing makes the pulse jump, when sweating leaves the chest feeling wired, or when a normal day suddenly feels much harder than expected.
Simple food and fluid habits can help this layer. Salt to taste with meals, broth, mineral rich animal foods, and whole food potassium sources can support steadier output. Plain water alone is not always enough, especially in heat or after heavy sweating.
Stable Meals
Big swings in food can make the chest feel rough even when no major disease is present. A sugary breakfast, constant snacking, or a long fast followed by a huge late meal can leave pulse and mood much less settled.
Many people do better with one to three solid meals and little or no grazing between them. Meals built from ruminant meat, eggs, fish, butter, tallow, and other animal foods often hold much better than low fat snack foods built on grains and sugar.
Animal foods also offer better nutrient density and bioavailability, which means the body can usually use those nutrients more easily. That can matter when the goal is steady energy, calmer pulse, and fewer swings through the day.
Fiber gets sold as a major fix for heart and hunger, yet fiber is non essential and often overpraised. Many high fiber plant foods also bring antinutrients and defense chemicals, which some people handle poorly, so steady protein, animal fat, and minerals often help more than bran cereal or fortified grain products.
Daily Pressures
Stress Load

The heart responds quickly to stress signals, even when the person does not notice the load building at first. Poor sleep, late eating, high tension, and nonstop stimulation can keep pulse and pressure high long after the day should have settled down.
A person may wake tired, feel revved after dark, or notice that the chest feels thumpy after a hard day. That often reflects stress chemistry and poor recovery more than true strength or better fitness.
Borrowed energy can hide this problem for a while, but it does not solve it. The body may keep pushing with stress hormones until the pulse, breath, and sleep all start to feel less steady.
Stimulant Push
Caffeine is more mixed than simple advice suggests, because moderate intake is tolerated by many people while high doses can cause trouble.
Reviews do not show a clear rise in atrial fibrillation risk at usual intake in many settings, but results vary and sensitivity differs from person to person (Caldeira et al., 2013; Surma et al., 2023).
A newer review notes that caffeine responses vary and that risk can rise in more vulnerable settings, especially when high doses are involved (Hamad, 2024). That means caffeine can feel fine one week and awful the next when sleep, food, fluids, and stress all shift at once.
Nicotine and repeated stress can do much the same thing, because they push output without building the base. A chest that feels more stable after rest, food, and minerals often gives a clue that the issue was strain rather than true stamina.
Recovery Clues
The body often gives warning signs before a clear problem gets named. Getting winded too easily, feeling a pounding pulse with small effort, noticing flutter feelings, or taking too long to recover after stress all deserve respect.
A pulse that stays high long after effort can be one of the clearest clues. That pattern may reflect under recovery, poor sleep, dehydration, low food intake, too much stimulant use, or a base that has not been built well.
Standing up and feeling the heart race can be another useful clue. Low fluid volume, low sodium, under eating, poor sleep, and high stress can all feed into that feeling even before a more serious condition gets ruled in or ruled out.
Steady Support
Food First
The heart needs fuel that feels steady, not dramatic, and that usually points back to simple whole foods. Meals based on ruminant meat, eggs, shellfish, broth, butter, and full fat dairy if tolerated can give protein, fat, copper, and minerals in a compact form.
That style of eating also avoids many foods that tend to make appetite, energy, and pulse feel less settled. Seed oils, ultra processed foods, fortified products, and grain based snack foods often push the body toward swings rather than steadiness.
A simple day can look like eggs cooked in butter for the first meal, beef patties with broth for the next meal, and sardines or lamb with a small side of tolerated fruit later on. Fewer meals often work better than endless grazing because the body gets a full signal rather than a stream of small hits.
Easy Movement
Easy walking is one of the best tools for daily heart support because it builds capacity without shocking the system. Research on exercise related heart change supports the value of steady training for better heart function and energy handling (Fulghum and Hill, 2018; Kolwicz, 2018).
Many people improve more with easy, repeatable work than with random hard sessions that leave recovery worse. A calmer breath at the same pace and faster pulse recovery after effort are both useful signs that the base is improving.
Hard intervals can help later, but they usually fit better after the base is there. A weak base plus hard work often feels like a shock rather than useful training.
Care Signals
Some signs need prompt medical care rather than guesswork at home. Chest pressure, fainting, near fainting, new severe shortness of breath, or a sustained irregular rhythm should never be brushed aside.
Frequent new palpitations deserve a real check as well, especially when they are getting worse or showing up with weakness, dizziness, or breathlessness. A basic workup can rule out serious problems and reduce guesswork before small issues become larger ones.
Before changing your diet, supplements, or health routine, talk with a licensed healthcare professional. For any health concerns or questions about a medical condition, get guidance from a physician or another appropriately trained clinician.
Research
Balaban, R.S. (2012) ‘Perspectives on: SGP symposium on mitochondrial physiology and medicine: metabolic homeostasis of the heart’, Journal of General Physiology, 139(6), pp. 407–414. Available at: https://doi.org/10.1085/jgp.201210783
Li, Y., Röder, F., Wanderoy, S., Bergmann, M., Grune, J., Blume, J., Mangels, N., Terjung, D., Meier, M., Möller, J.-M., Djonov, V. and Flögel, U. (2023) ‘Giant mitochondria in cardiomyocytes’, Basic Research in Cardiology, 118, article 39. Available at: https://doi.org/10.1007/s00395-023-01005-y
Stanley, W.C., Recchia, F.A. and Lopaschuk, G.D. (2005) ‘Myocardial substrate metabolism in the normal and failing heart’, Physiological Reviews, 85(3), pp. 1093–1129. Available at: https://doi.org/10.1152/physrev.00006.2004
Lopaschuk, G.D., Karwi, Q.G., Tian, R., Wende, A.R. and Abel, E.D. (2021) ‘Cardiac energy metabolism in heart failure’, Circulation Research, 128(10), pp. 1487–1513. Available at: https://doi.org/10.1161/CIRCRESAHA.121.318241
Negru, A.G., Pastorcici, A., Crisan, S., Cismaru, G., Popescu, F.G. and Luca, C.T. (2022) ‘The role of hypomagnesemia in cardiac arrhythmias: a clinical perspective’, Biomedicines, 10(10), article 2356. Available at: https://doi.org/10.3390/biomedicines10102356
Weiss, J.N., Qu, Z. and Shivkumar, K. (2017) ‘Electrophysiology of hypokalemia and hyperkalemia’, Circulation: Arrhythmia and Electrophysiology, 10(3), e004667. Available at: https://doi.org/10.1161/CIRCEP.116.004667
Tazmini, K., Frisk, M., Lewalle, A., Laasmaa, M., Morotti, S., Lipsett, D.B., Manfra, O., Skogestad, J., Aronsen, J.M., Sejersted, O.M., Sjaastad, I., Edwards, A.G., Grandi, E., Niederer, S.A., Øie, E. and Louch, W.E. (2020) ‘Hypokalemia promotes arrhythmia by distinct mechanisms in atrial and ventricular myocytes’, Circulation Research, 126(7), pp. 889–906. Available at: https://doi.org/10.1161/CIRCRESAHA.119.315641
Caldeira, D., Martins, C., Alves, L.B., Pereira, H., Ferreira, J.J. and Costa, J. (2013) ‘Caffeine does not increase the risk of atrial fibrillation: a systematic review and meta-analysis of observational studies’, Heart, 99(19), pp. 1383–1389. Available at: https://doi.org/10.1136/heartjnl-2013-303950
Surma, S., Romańczyk, M., Filipiak, K.J. and Lip, G.Y.H. (2023) ‘Coffee and cardiac arrhythmias: up-date review of the literature and clinical studies’, Cardiology Journal, 30(4), pp. 654–667. Available at: https://doi.org/10.5603/CJ.a2022.0068
Hamad, A.K.S. (2024) ‘Caffeine and arrhythmias: a critical analysis of cardiovascular responses and arrhythmia susceptibility’, Journal of the Saudi Heart Association, 36(4), pp. 335–348. Available at: https://doi.org/10.37616/2212-5043.1402
Fulghum, K. and Hill, B.G. (2018) ‘Metabolic mechanisms of exercise-induced cardiac remodeling’, Frontiers in Cardiovascular Medicine, 5, article 127. Available at: https://doi.org/10.3389/fcvm.2018.00127
Kolwicz Jr, S.C. (2018) ‘An “exercise” in cardiac metabolism’, Frontiers in Cardiovascular Medicine, 5, article 66. Available at: https://doi.org/10.3389/fcvm.2018.00066
Brown, D.A., Perry, J.B., Allen, M.E., Sabbah, H.N., Stauffer, B.L., Shaikh, S.R., Cleland, J.G.F., Colucci, W.S., Butler, J., Voors, A.A., Anker, S.D., Pitt, B., Pieske, B., Filippatos, G., Greene, S.J. and Gheorghiade, M. (2017) ‘Mitochondrial function as a therapeutic target in heart failure’, Nature Reviews Cardiology, 14, pp. 238–250. Available at: https://doi.org/10.1038/nrcardio.2016.203
Fulghum, K. and Hill, B.G. (2018) ‘Metabolic mechanisms of exercise-induced cardiac remodeling’, Frontiers in Cardiovascular Medicine, 5, article 127. Available at: https://doi.org/10.3389/fcvm.2018.00127
Fukushima, A., Lopaschuk, G.D. and Stanley, W.C. (2016) ‘Cardiac fatty acid oxidation in heart failure associated with obesity and diabetes’, Biochimica et Biophysica Acta (BBA) – Molecular and Cell Biology of Lipids, 1861(10), pp. 1525–1534. Available at: https://doi.org/10.1016/j.bbalip.2016.03.020
Heggermont, W.A., Papageorgiou, A.-P., Heymans, S. and van Bilsen, M. (2016) ‘Metabolic support for the heart: complementary therapy for heart failure?’, European Journal of Heart Failure, 18(12), pp. 1420–1429. Available at: https://doi.org/10.1002/ejhf.678
Karwi, Q.G., Uddin, G.M., Ho, K.L. and Lopaschuk, G.D. (2018) ‘Loss of metabolic flexibility in the failing heart’, Frontiers in Cardiovascular Medicine, 5, article 68. Available at: https://doi.org/10.3389/fcvm.2018.00068
Kolwicz Jr, S.C., Purohit, S. and Tian, R. (2013) ‘Cardiac metabolism and its interactions with contraction, growth, and survival of cardiomyocytes’, Circulation Research, 113(5), pp. 603–616. Available at: https://doi.org/10.1161/CIRCRESAHA.113.302095
Nagoshi, T., Yoshimura, M., Rosano, G.M.C., Lopaschuk, G.D. and Mochizuki, S. (2011) ‘Optimization of cardiac metabolism in heart failure’, Current Pharmaceutical Design, 17(35), pp. 3846–3853. Available at: https://doi.org/10.2174/138161211798357827
Sejersted, O.M. and Sjøgaard, G. (2000) ‘Dynamics and consequences of potassium shifts in skeletal muscle and heart during exercise’, Physiological Reviews, 80(4), pp. 1411–1481. Available at: https://doi.org/10.1152/physrev.2000.80.4.1411
Skogestad, J. and Aronsen, J.M. (2018) ‘Hypokalemia-induced arrhythmias and heart failure: new insights and implications for therapy’, Frontiers in Physiology, 9, article 1500. Available at: https://doi.org/10.3389/fphys.2018.01500
Zuchinali, P., Ribeiro, P.A.B., Pimentel, M., da Rosa, P.R., Zimerman, L.I. and Rohde, L.E. (2016) ‘Effect of caffeine on ventricular arrhythmia: a systematic review and meta-analysis of experimental and clinical studies’, Europace, 18(2), pp. 257–266. Available at: https://doi.org/10.1093/europace/euv261